The Current State of Health in the US
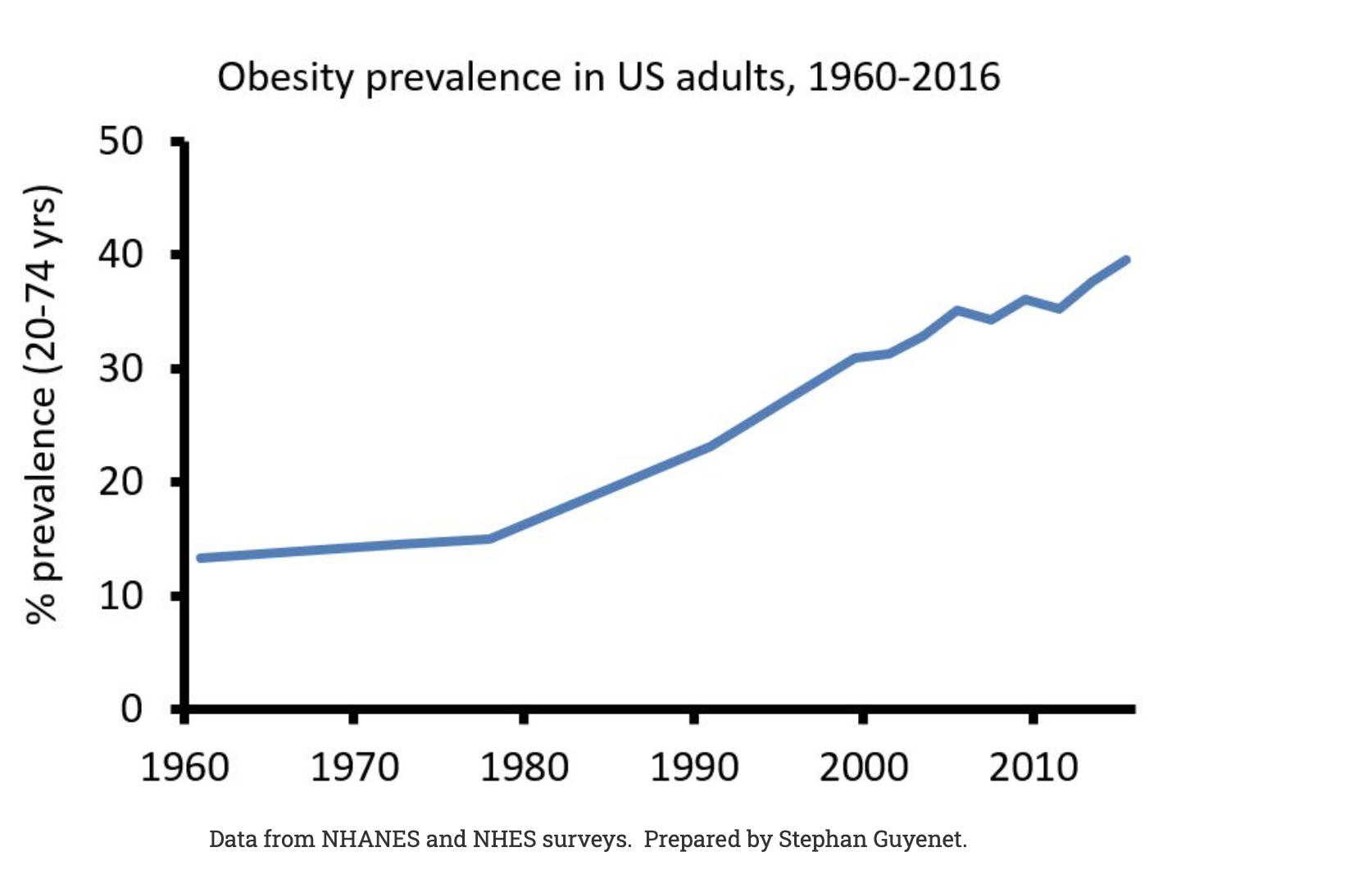
The obesity rate has increased nearly 300% since 1960.

7 in 10 adults are now overweight or obese

6 in 10 adults have a chronic disease and 4 in 10 have two or more.
Since these changes happened in the space of a single lifetime, they cannot be attributed to genetics.
So what changed?
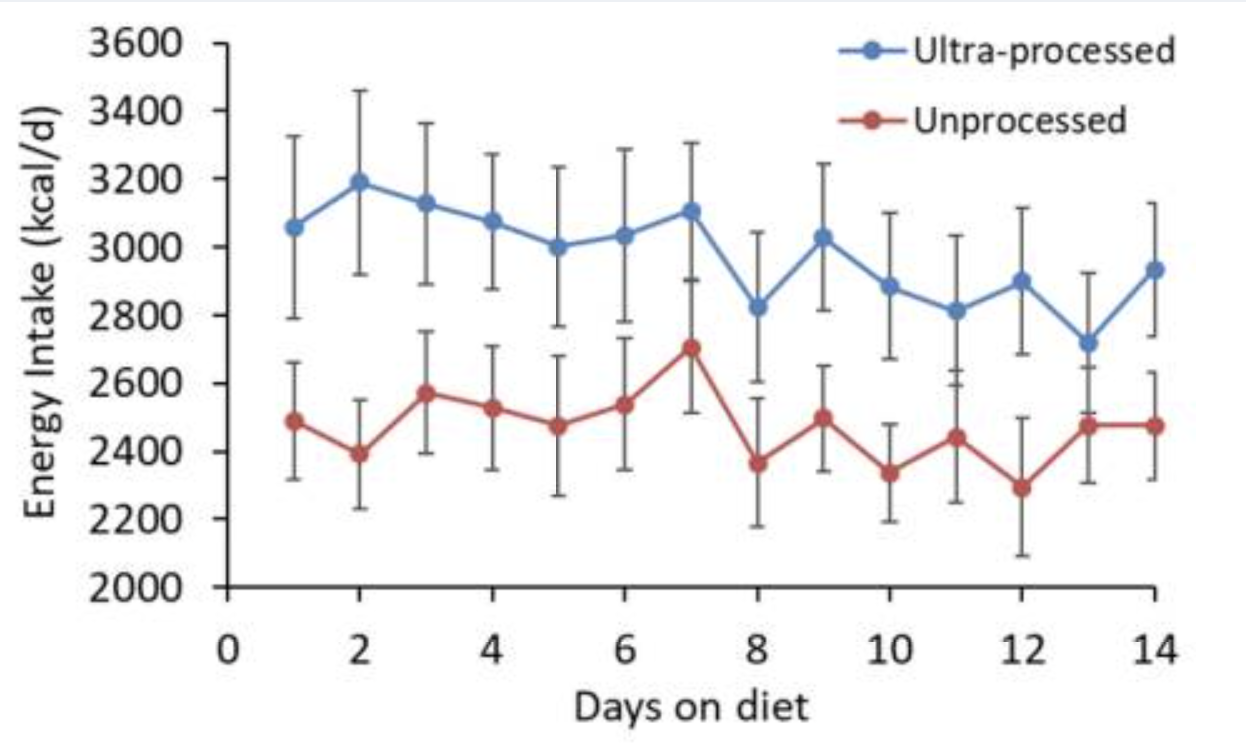
In the US, these foods now make up 60% of calories consumed.
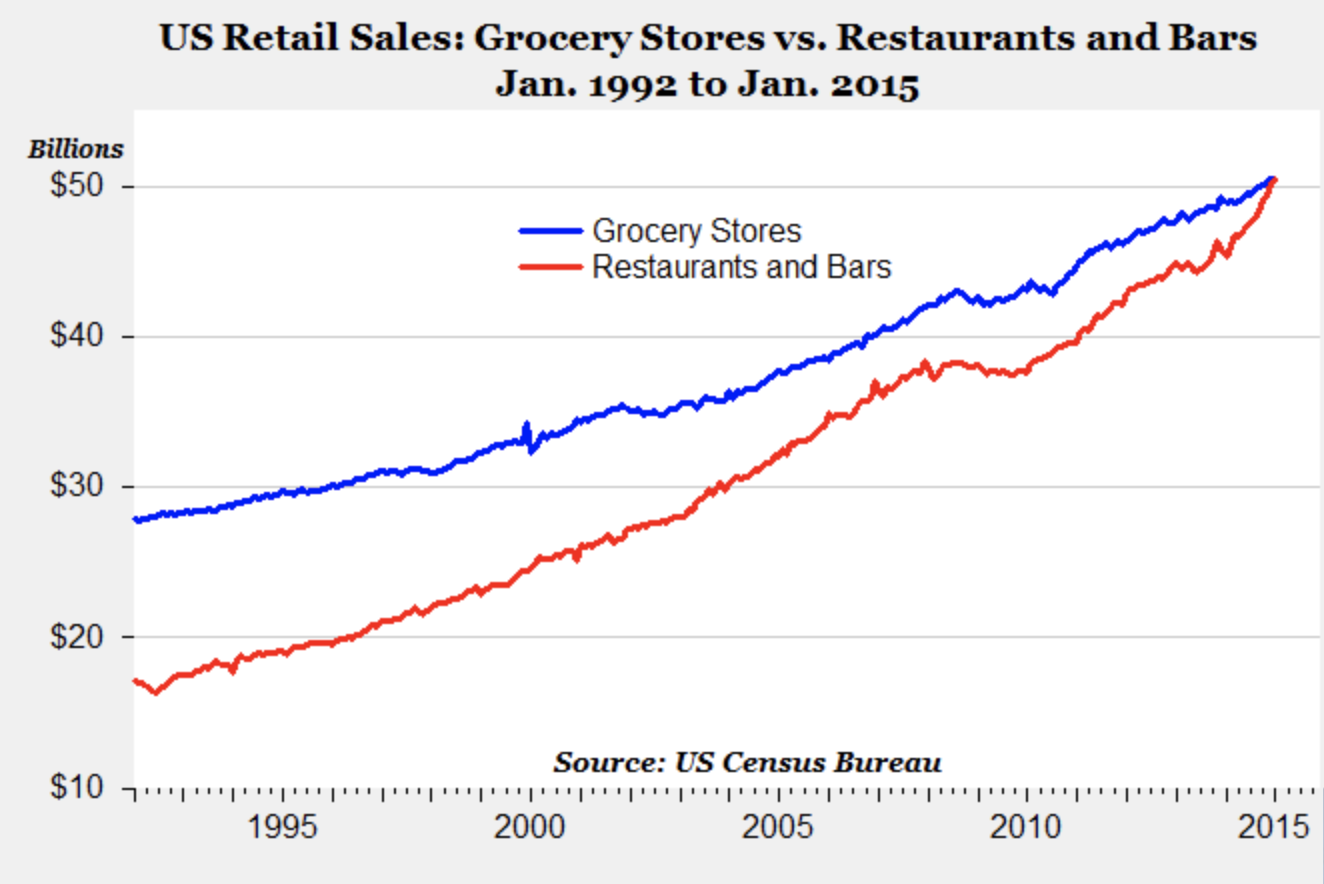
People who eat out consume 200 more calories per day than when they eat at home. Restaurant meals now make up 20% of total daily calories consumed in the US. These meals are often loaded with sodium, fat and added sugar. One study showed that fewer than 0.1% of restaurant meals consumed were of “ideal quality” according to American Heart Association.
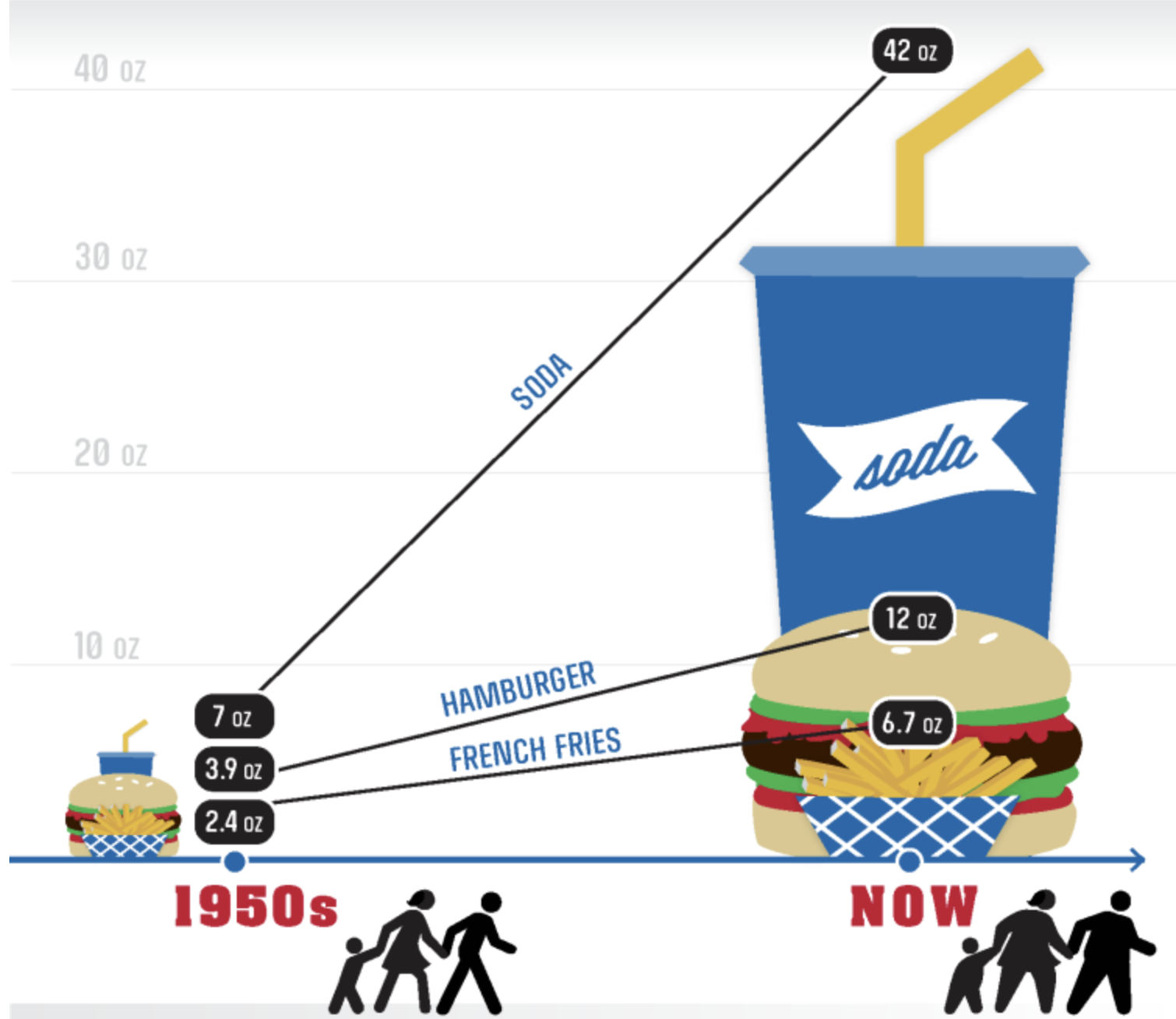
Between 1977 and 1996, food portion sizes increased both inside and outside the home for all categories except pizza.
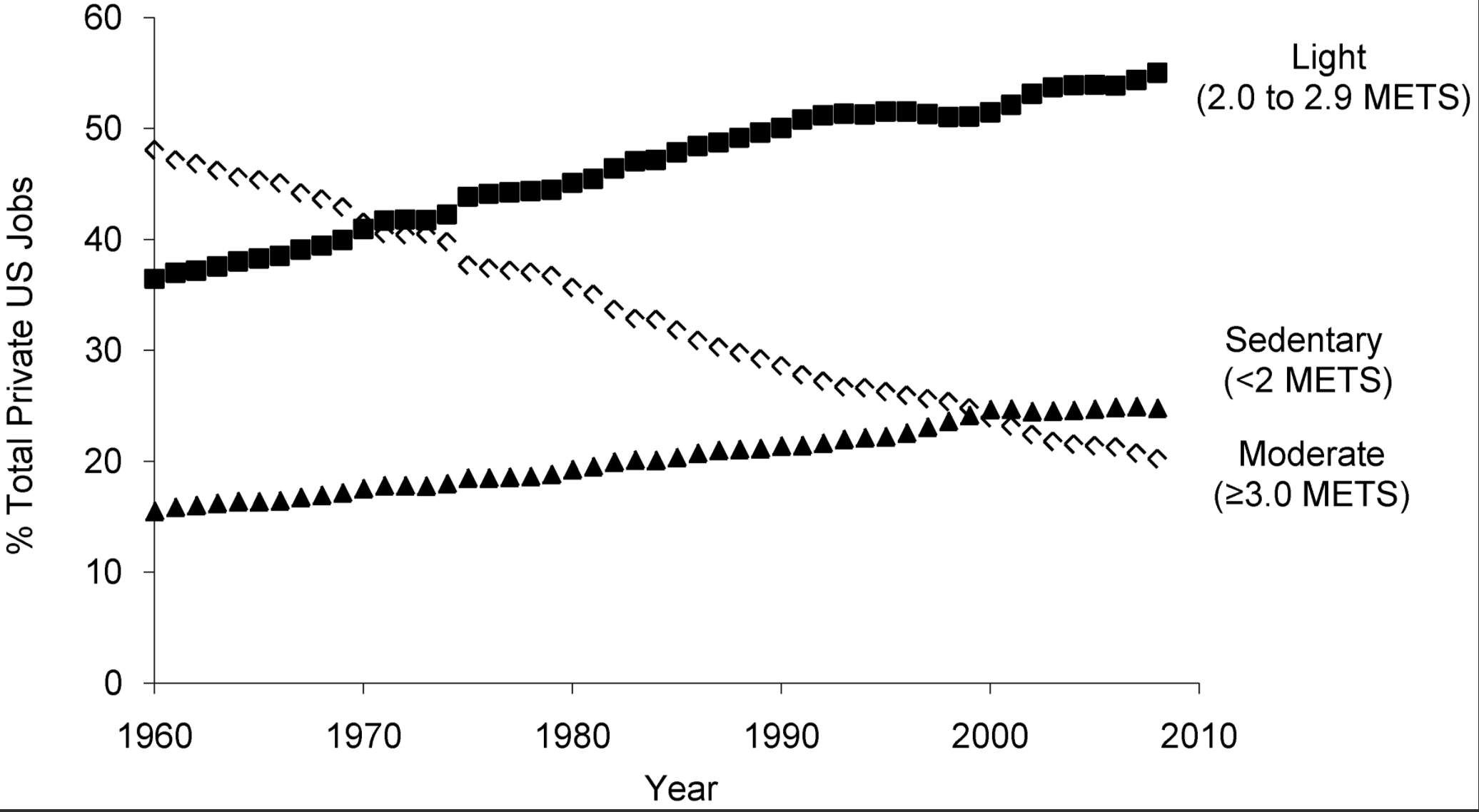
Since 1960 moderate activity jobs have decreased while sedentary and light activity jobs have increased. This accounts for over 100 fewer calories burned per day.
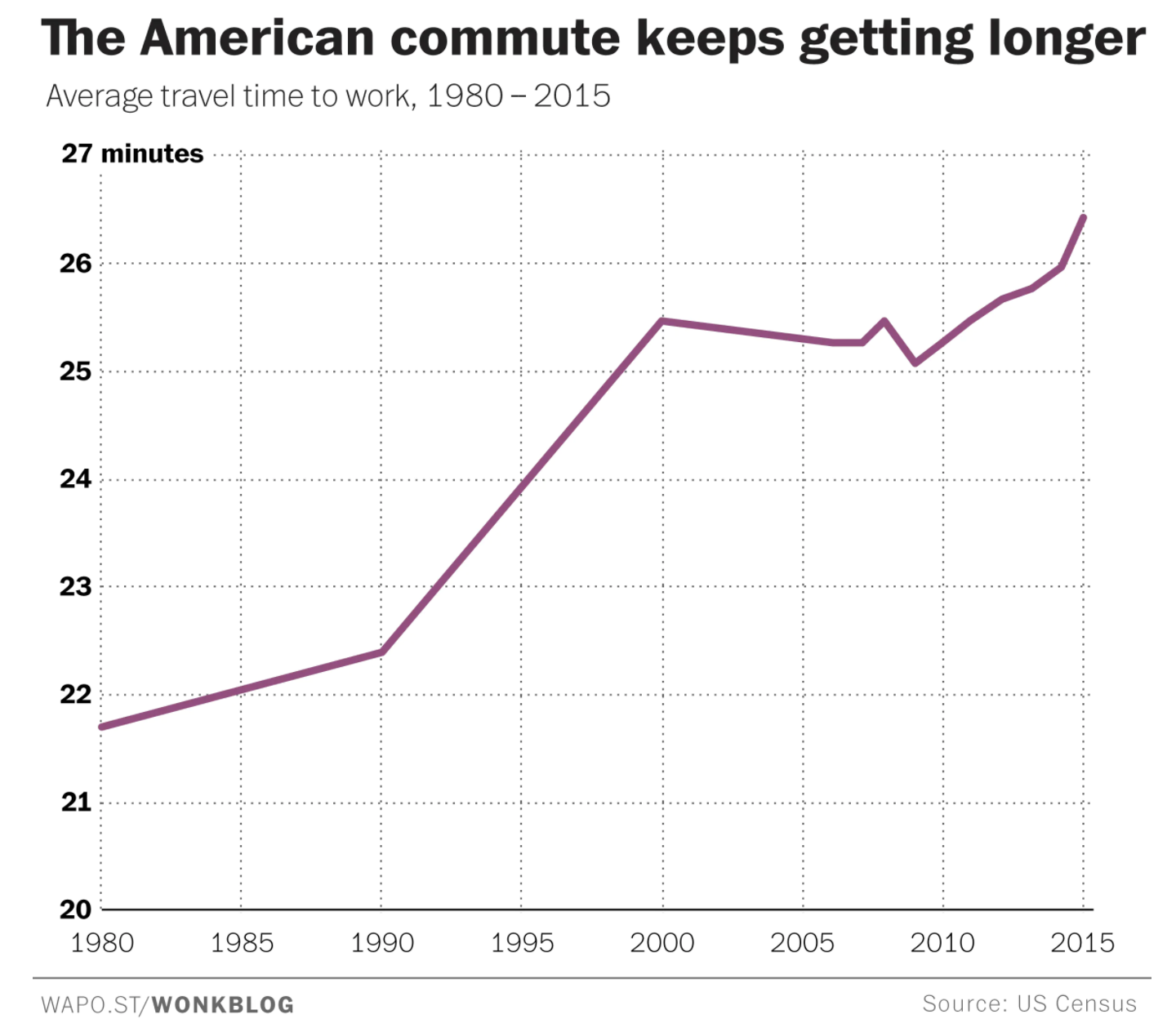
Average commute time has increased significantly since 1980 and extreme commutes are the fastest growing type.
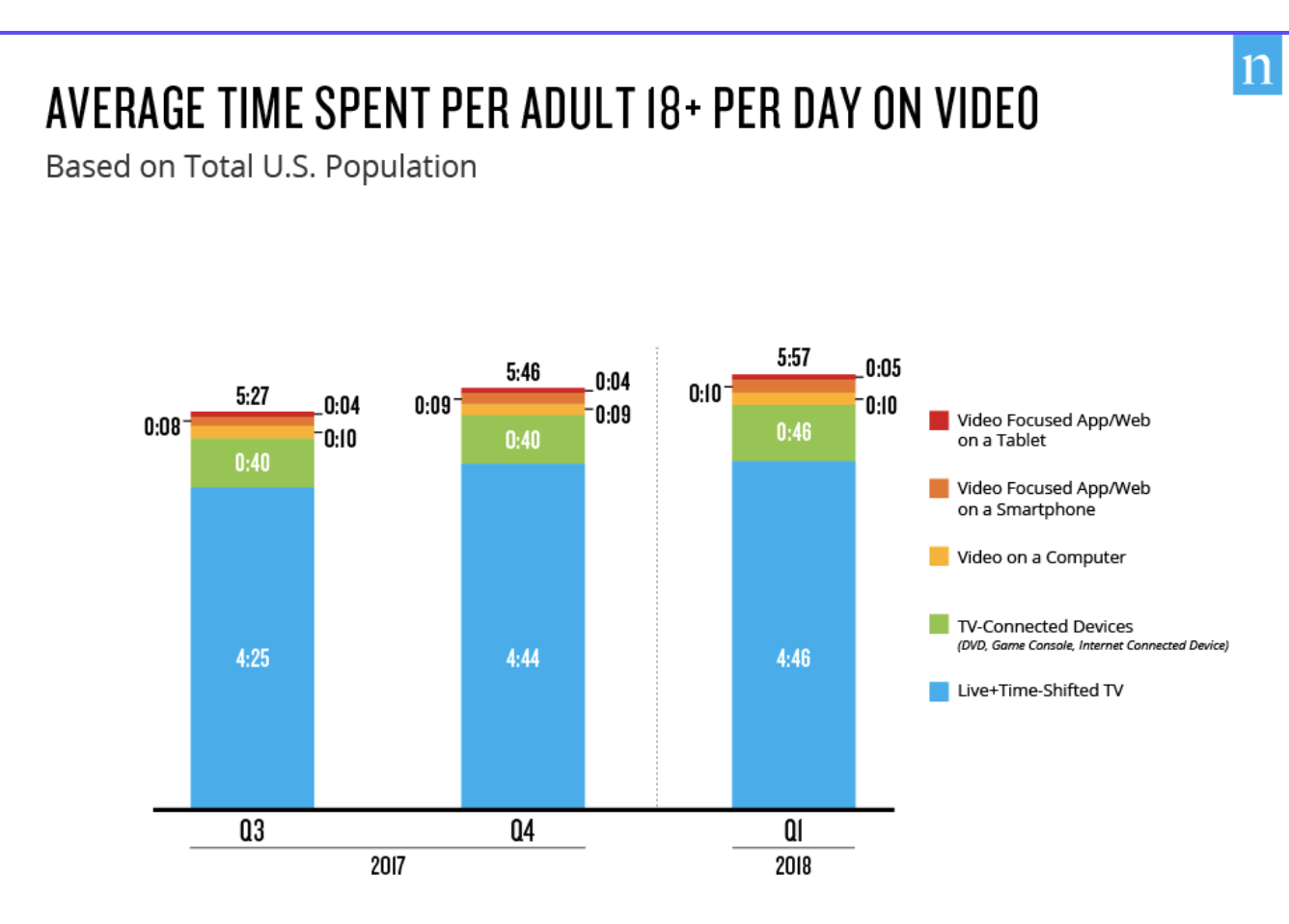
U.S. adults spend almost 6 hours a day watching video. Average time spent on all media (including social media, web, and gaming) is now over 11 hours per day.
We are also less rested and more stressed than in the past. These issues alter our hormonal environment in ways that make it more difficult to eat healthily and exercise.
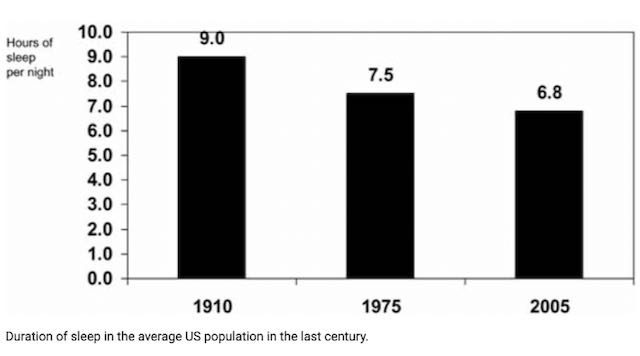
Sleep restriction has been found to significantly increase subjective hunger and calorie intake in multiple studies. Decreased sleep is associated with increased obesity, diabetes, and cardiovascular risk.
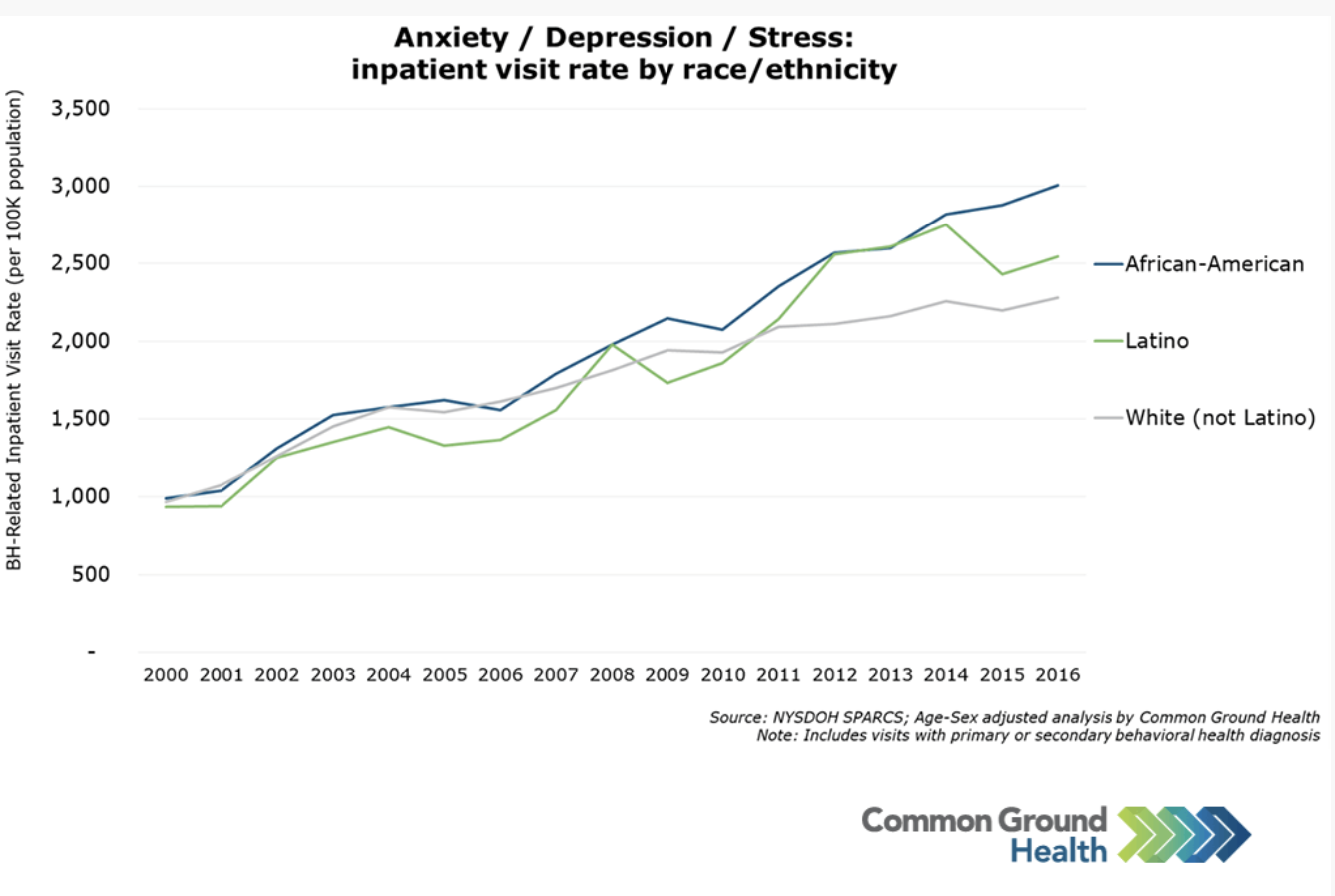
Chronic stress ramps up appetite. Individuals with more stressors have been shown to have higher insulin levels and lower fat oxidation.
The central problem is our environment.
The modern world is an environment that encourages inactivity and overconsumption. It’s an environment where obesity and chronic disease have become the new normal.
Behavioral interventions offer a proven solution.
- The US Preventative Service Task Force recommends that clinicians refer adults with a body mass index (BMI) of 30 or higher to intensive, multicomponent behavioral interventions.
- Behavioral interventions empower people with skills to overcome environmental obstacles.
- These programs help people to set personalized goals to gradually improve diet, and physical activity and build sustainable healthy habits for life.
What are the core components of behavioral interventions?
Decades of research have shown that successful programs have 4 common features.
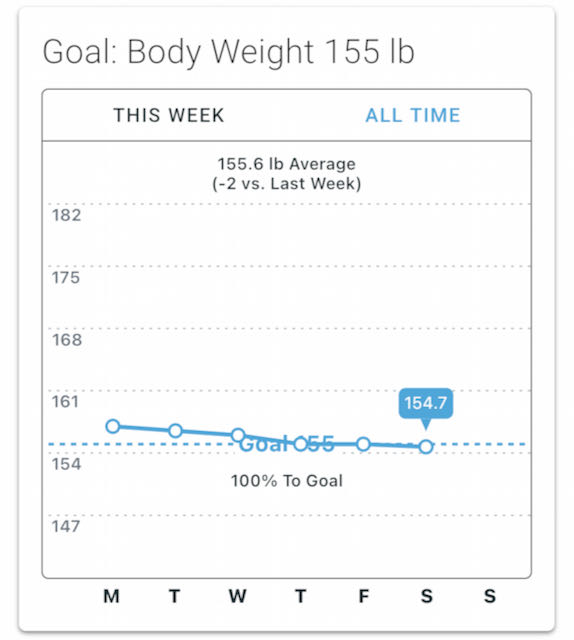
Having participants set a health goal (like a weight loss amount) is a critical foundational element in successful programs. This has been cited as a success driver in meta-analysis of both weight loss and diabetes prevention programs. While participants may choose to change their goal at some point, setting a goal initially indicates a starting point for their journey and helps them consider whether their actions are consistent with the goal they’ve selected.
Clients can set health goals for weight, body fat and circumferences. They are then able to set behavior targets (with input from their coach) to help them achieve these goals.
A curriculum on how to eat, exercise and sustain healthy habits in a challenging environment is another foundational element in successful programs. One of the most widely studied behavior change curriculas is The Diabetes Prevention Program funded by NIH in 1996. Participants in this program showed a 58% reduction in the rate of diabetes in the first 3 years after completion. Follow up studies demonstrated long term behavior change with lower diabetes risk in participants 15 years after program completion. This program is now delivered nationally at over 1500 sites, and the curriculum has been adapted as the basis of many other behavior change programs.
The coaching interface comes with evidence based lessons on nutrition, exercise, health, and behavior change. These cover core topics featured in the National Diabetes Prevention Program curricula, but are condensed to be engaging like social media.
To maximize flexibility, coaches can easily create their own lessons by uploading images or can link to videos, podcasts and other resources on the web.
Studies have repeatedly shown that people who track diet, exercise and weight are more likely to reach their health goals. Tracking calories eaten, or steps taken against daily targets provides feedback on whether a client is moving in the direction of a weight loss destination. The act of tracking also creates an awareness that causes people to improve their choices. Studies have repeatedly shown a positive relationship between the frequency of tracking and the amount of weight loss. One study with nearly 1700 participants found that people who kept a daily food diary had double the weight loss of people who didn’t track their food.
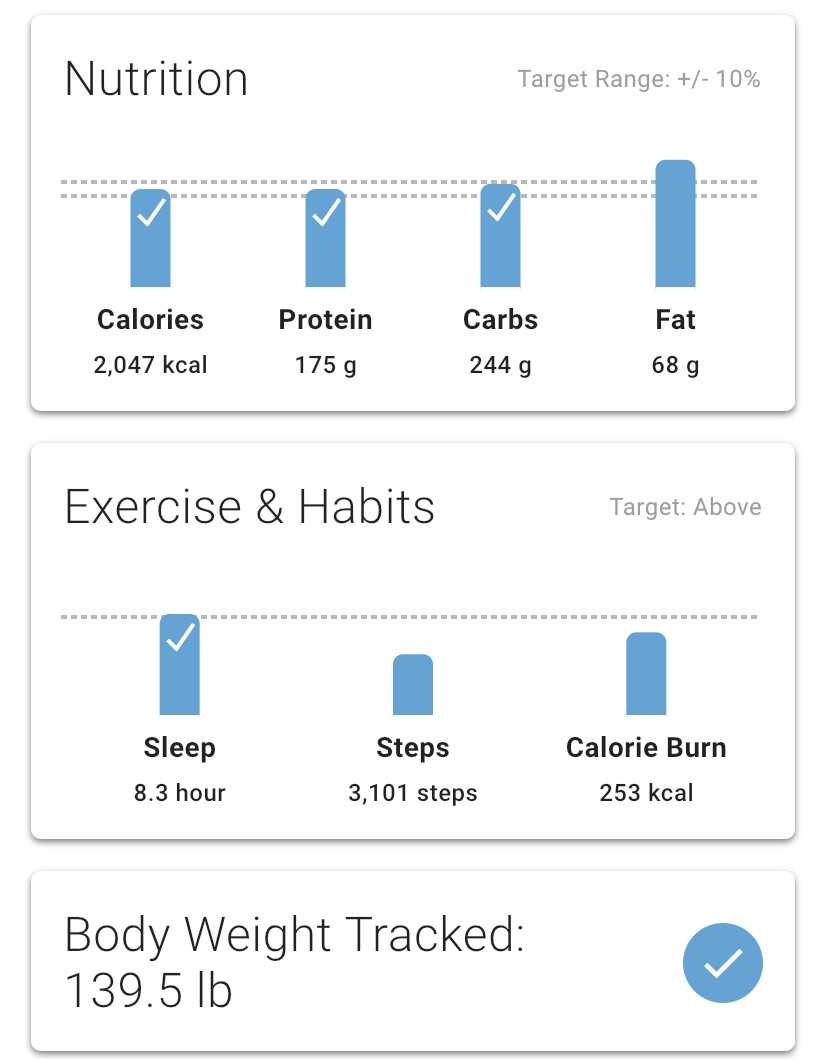
Participants can self-monitor nutrition, steps, calorie burn, sleep, weight, and body fat through any app, or connected device that integrates with Apple Health or Google Fit.
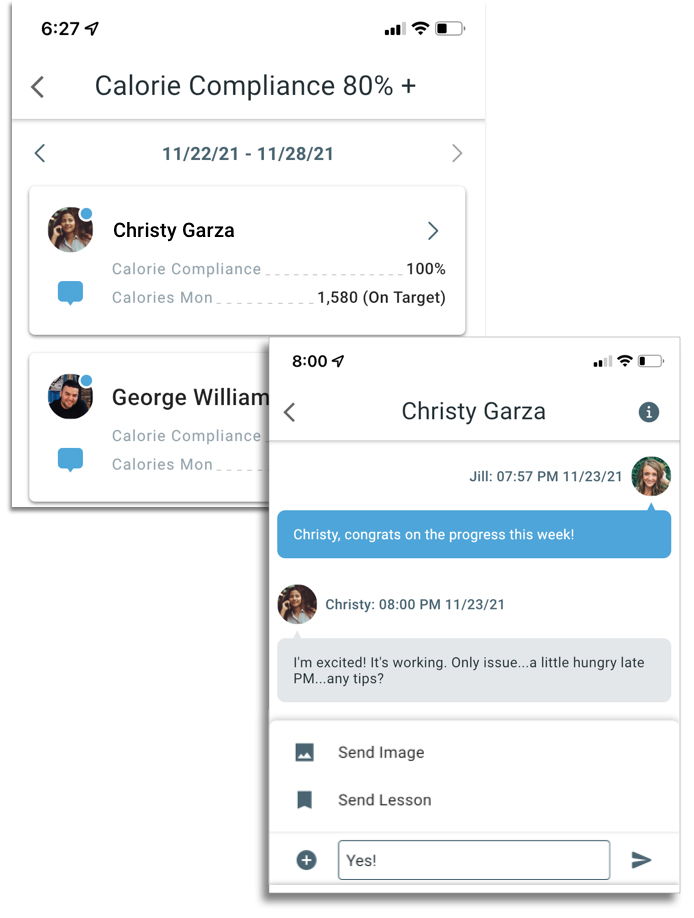
A review of 39 clinical weight loss trials noted that feedback and support from coaches was a common component in successful programs. Personalized coaching enhances the effectiveness of all of the other behavior change components. Coaches provide an extra layer of accountability for goals, they can explain concepts in a curriculum, and a major way they can impact success is by encouraging self-monitoring and helping to problem solve. A weight loss study with 210 participants showed that a daily feedback message delivered remotely enhanced adherence to self-monitoring and this more frequent self-monitoring led to improved weight loss. A review of 12 weight loss studies found that participants who received personalized coaching feedback on their behaviors (like food tracking) were twice as likely to reach 5% weight loss as those who didn’t receive it.
Health Mentor was built to enable this type of coaching. Coaches can efficiently monitor diet, sleep, and exercise for every client from a single dashboard. With a single tap they can filter to see lists of clients who are meeting or struggling with behavior goals. With an additional tap they can message clients to encourage self-monitoring, and provide accountability. When needed, they can follow up with evidence-based lessons from the integrated content library as easily as sending an emoji.